  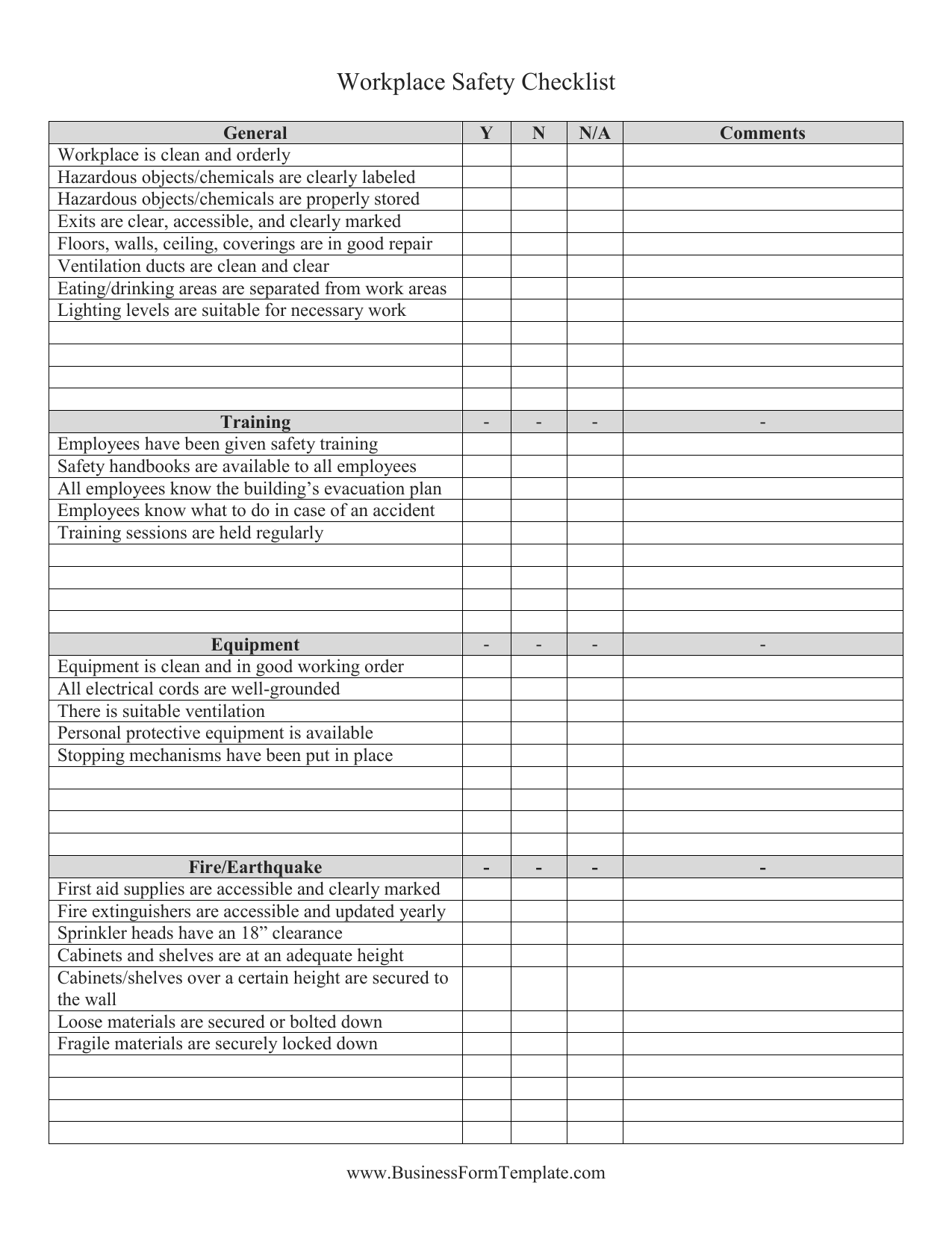
Perioperative care teams should acknowledge that fiber-optic light cables are a potential hazard associated with fire safety and use GloShield to mitigate this risk.Ĥ.4 – “ Based on results of fire prevention assessment, implement the necessary interventions (preventive measures in Section 4.6). The following are guidelines in the AORN 2021 Edition of Guidelines for Perioperative Practice pertaining to fire safety:Ĥ.1 – “ Identify potential hazards associated with fire safety and establish safe practices for communication, prevention, suppression, and evacuation.” Read below to learn how GloShield aligns with TJC standards and AORN guidelines. GloShield is a single-use surgical safety device designed to mitigate the fire risk associated with fiber-optic light cables as an ignition source. An often overlooked aspect of perioperative fire safety is fiber-optic light cables as an ignition source. One of the most important topics covered in these guidelines is perioperative Fire Safety listed under Environment of Care. AORN has published its 2021 Edition of Guidelines for Perioperative Practice, and it’s filled with over 1,000 pages of incredible, in-depth insights on how to provide the best perioperative care. The Joint Commission’s surveys are always around the corner, where hospitals are expected to show the quality of the care they provide according to their Life Safety & Environment of Care Document List and Review Tool. “This also give us the opportunity to ensure that our standards and elements of performance are effective and contemporary.The Joint Commission and AORN are two leading institutions that are working hard to create a higher standard of care in hospitals. 
“The Joint Commission’s Emergency Management Committee continues meeting with organizations after disaster events to glean important information to share with the field through our Environment of Care News and ongoing communications,” he adds. “Establishing an unidentified victims process is also a good start, as it the ability to share that information within an hour of a disaster event.” “For example, in Florida, a county Office of Emergency Management met with utilities and other emergency support functions to determine hospitals and PSAPS are the first to receive power restoration,” he says. Jim Kendig, TJC’s field director of Life Safety Code surveyors, says it’s critical that hospitals customize the checklist for their needs by examining the relationships they establish in the community, and at the regional and state levels. It should be noted that the checklist isn’t hurricane-specific. It aligns with the accreditor’s Emergency Management standards, covers both clinical and environmental issues, and addresses crucial post-disaster elements that need addressing before reopening. Department of Health & Human Services’ Office of the Assistant Secretary for Preparedness and Response. While the timing of these two events were coincidental, providers should to take time to go over the checklist and their emergency plans in general.Ī TJC workgroup developed the checklist at the request of the U.S. On the same day, The Joint Commission (TJC) published a new Emergency Management Health Care Environment Checklist on its website, which helps healthcare organizations reopening their facilities after a disaster. On October 10, Hurricane Michael made landfall in Florida. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
